Physical Therapy for Urinary Incontinence
What is Urinary Incontinence?
Urinary Incontinence (UI), or the leakage of urine, affects an estimated 13 million Americans. Both men and women of all ages can experience UI that can make them feel ashamed and isolated.
Innovations in therapy have made UI much easier to treat than in the past. Still, millions of individuals continue to suffer the discomfort and inconvenience of UI. Despite its annual cost of $15 billion dollars, most individuals do not seek help for UI, primarily due to embarrassment.
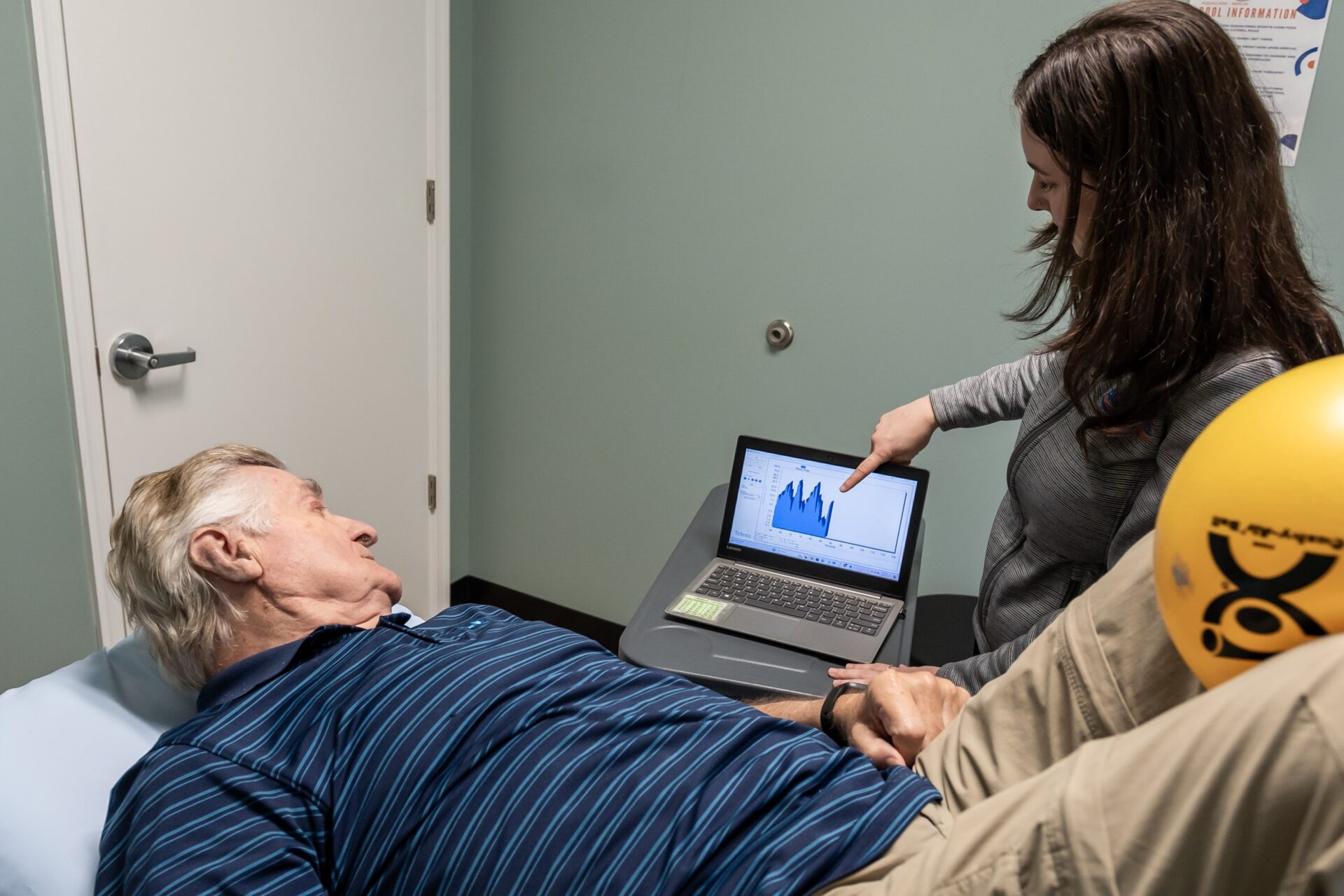
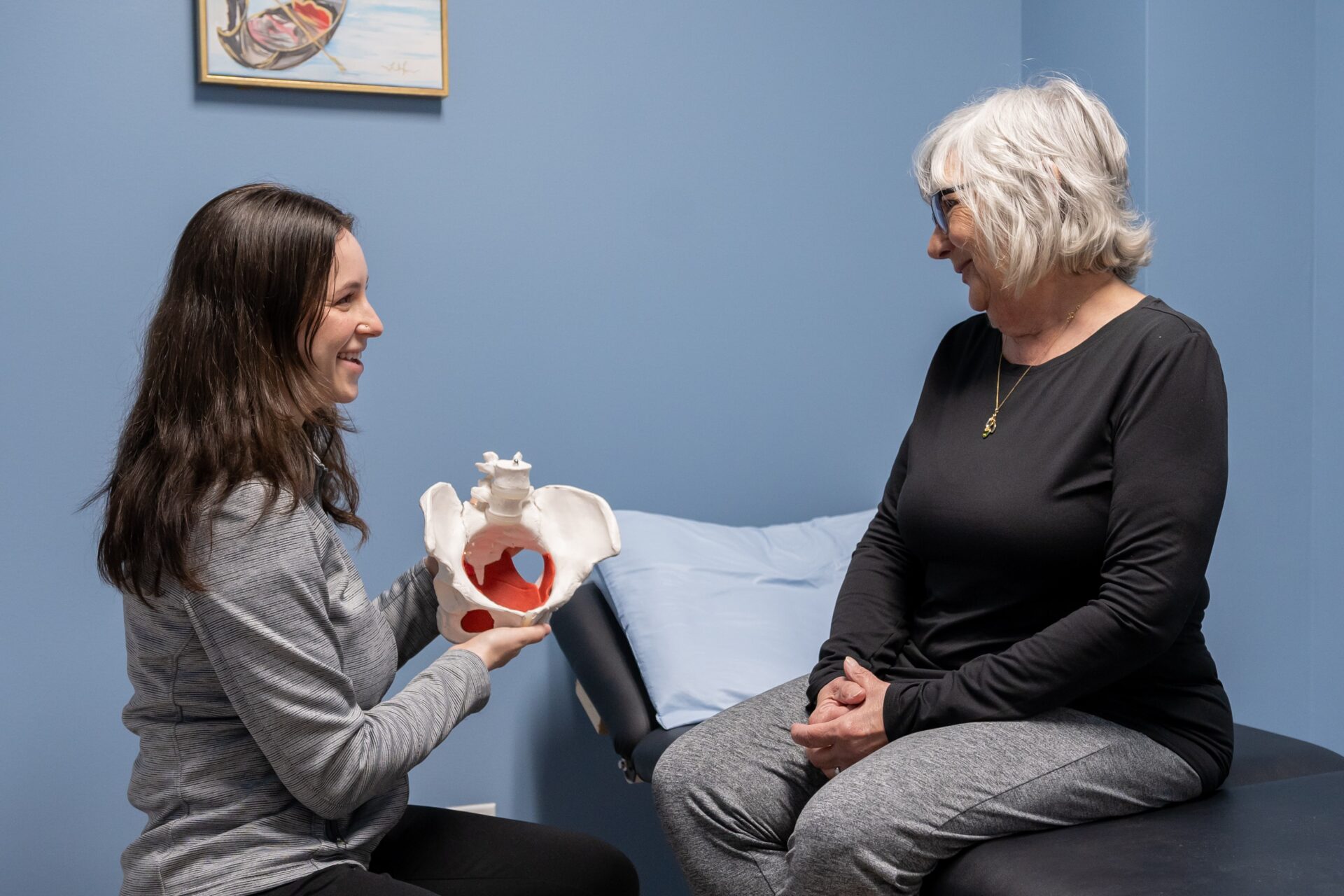
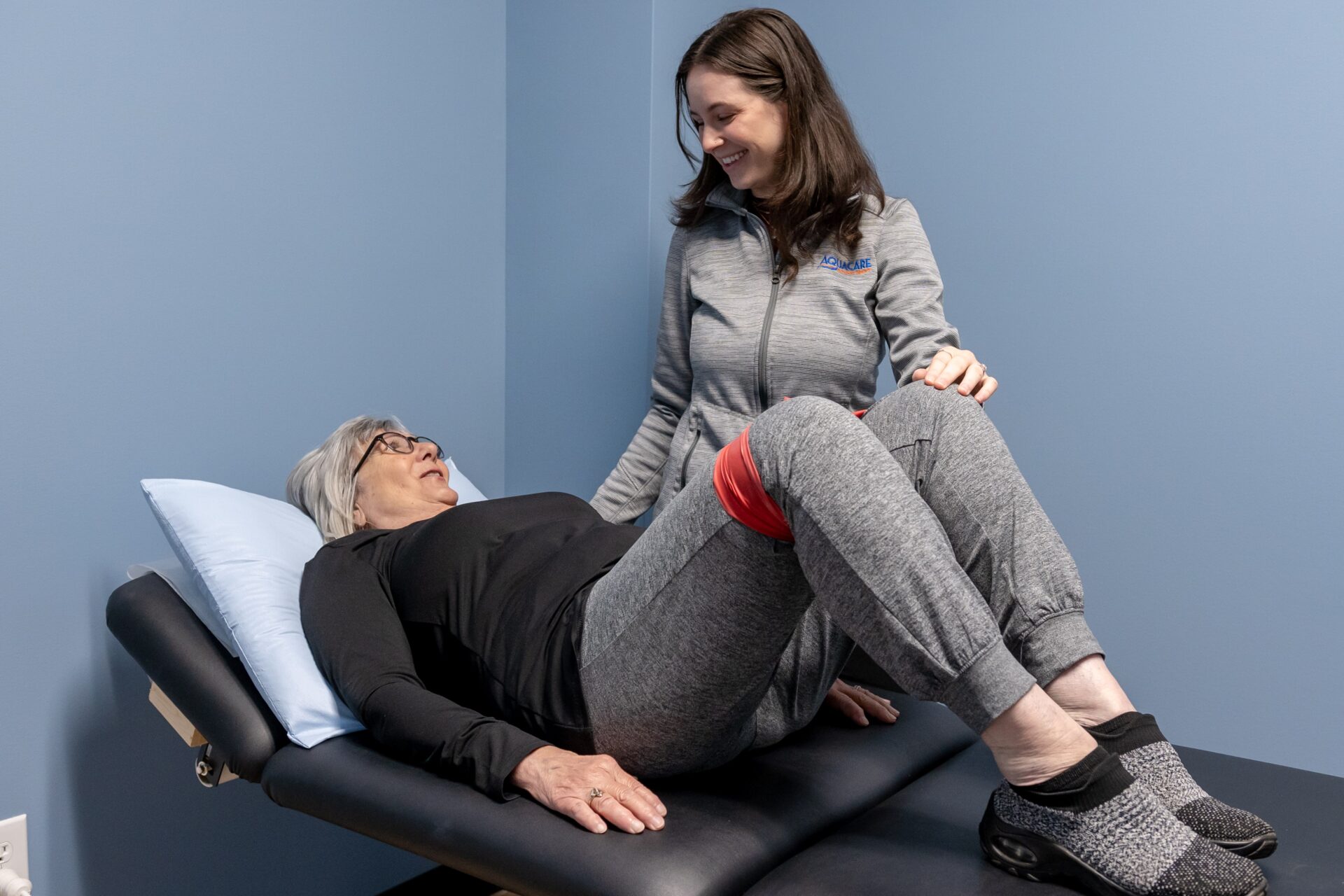
Don’t be embarrassed by your leaks – we can help. Our pelvic floor specialists have proven methods to help you improve your core and reduce leaks. Call one of our locations to schedule your appointment with a urinary incontinence specialist today.